By Mari-An Santos
Four young Filipino nurses have been speaking to Mari-An Santos about their experiences of working in NHS hospital Covid-19 wards and in intensive therapy units (ITUs). Their ages range between 27 and 31 and most of them have been in the UK for less than 5 years. As the UK’s coronavirus death toll passes 50,000, we would like to share their stories of working in the frontlines.
This fourth piece tells the story of Fatima Zaldua.
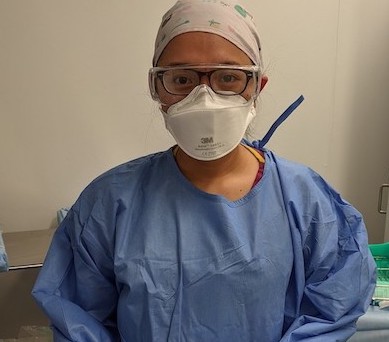
Fatima Zaldua, 27, is a theatre nurse in Orpington. She has been working in the UK since October 2015. She had been keeping an eye on cases as Covid-19 spread in China and then Italy and Spain. When she heard about the first case in St. Thomas, “Oh no, this is the beginning,” she thought. “You could just feel it! It spread so quickly! You could see in the atmosphere at the hospital, you could see how scared your colleagues were.”
First lockdown fears
“It just all piles up. You were scared at home, you were scared at work, and you just didn’t know anything about the virus. We just knew that it would get really bad. You have this creeping feeling inside that you are going to be part of it, you can’t escape it, you are going to be right at the center where COVID is going to happen.”
She felt conflicted as cases steadily rose in March and the threat of the first lockdown was looming. “I thought a lockdown was a good idea because it seemed to be working a bit in Italy.
But if there was going to be a lockdown, I wasn’t going to be able to see my boyfriend. My support system, someone physically near me, it’s just him. I thought that was going to be tough. He’s been very supportive, because I had voiced my concerns to him as well, crying: ‘This is going to be hell!’
Preparing for redeployment
“When they said the lockdown was going to happen, and then [at work], the redeployment. I was very, very scared. I started preparing to be redeployed to the wards,” says Zaldua. “I had to brush up on my knowledge. I had to prepare myself. I tried learning about the machines, what the treatment was, markers that would indicate when the patient was getting worse. I started studying. I also prepared myself mentally.
Sometimes I felt really alone, but I managed to continue and do my job properly and be there for patients. That just gave me strength. I feel a much better person.
“I requested my manager: If I have to choose, send me to critical care. But in the end, they sent me to the ward. It was a Covid-19 ward for three weeks. I was lucky in the sense that I wasn’t handling a lot of Covid-19 patients for a long time. Only for three weeks. But not as bad as the critical care nurses.”
“What doesn’t kill you makes you stronger”
Now that the second wave is come, they are continuing to work on elective procedures because they are behind on the patients’ operations. “But that can change at any time,” she says.
“It changes your perspective, it just makes you very appreciative of all the things that you have, all the important things in your life. Family, they’ve always been there for me and they’re always going to support me. They are my number one priority,” she reflects. “It made me realise how, even if I don’t feel like it, I am actually a strong person. Sometimes I felt really alone, but I managed to continue and do my job properly and be there for the patients. That just gave me strength. I feel a much better person. Hypothetically, what doesn’t kill you makes you stronger. That’s what happened to me.”
Mari-An Santos is a freelance writer based in Manila. She recently finished a Joint Master’s degree in Women and Gender Studies from the University of Granada (Spain) and University of Lodz (Poland). Her thesis tackled Emotional Geographies of Ageing Filipina Migrant Workers in Valencia, Spain.